Introduction
Alopecia areata is an autoimmune condition in which the immune system targets hair follicles, leading to sudden, non-scarring hair loss. The condition primarily involves the skin and its hair follicles, but the biologic process is driven by immune signaling rather than by damage to the hair itself. In healthy skin, hair follicles cycle through phases of growth, regression, and rest in a controlled pattern. In alopecia areata, that cycle is interrupted when immune cells inappropriately attack follicles that are otherwise structurally intact. The result is a functional failure of hair production rather than permanent destruction of the follicle in most cases.
The disorder can affect any hair-bearing area, but it is most often recognized on the scalp. Because the follicle remains alive, the condition differs from scarring forms of alopecia in which follicles are replaced by fibrous tissue. Understanding alopecia areata requires looking at the hair follicle as a dynamic skin organ and at the immune system as the central driver of the abnormal process.
The Body Structures or Systems Involved
The main structure affected in alopecia areata is the hair follicle, a complex mini-organ embedded in the dermis. A follicle includes the hair bulb, which contains rapidly dividing matrix cells that generate the hair shaft, and the dermal papilla, a specialized cluster of connective tissue cells and blood vessels that helps regulate growth. Surrounding these structures are layers of epithelial cells that shape and protect the growing hair fiber.
In a healthy follicle, growth occurs in cycles. The anagen phase is the active growth stage, when matrix cells divide rapidly and produce the hair shaft. This is followed by the catagen phase, a short regression stage in which growth slows and the lower follicle shrinks. Finally, the follicle enters telogen, a resting stage before re-entering growth. This cycling is controlled by local signals in the skin, including growth factors, cytokines, and hormonal influences.
The immune system is the other major system involved. In alopecia areata, T lymphocytes, especially CD8+ cytotoxic T cells and CD4+ helper T cells, become active around the follicle. Cytokine signaling, particularly pathways involving interferon-gamma and interleukins, helps sustain the immune response. The condition is therefore not a problem of hair production alone; it is a disorder of immune privilege failure within a skin appendage.
How the Condition Develops
Alopecia areata develops when the immune system loses tolerance to the hair follicle. Under normal conditions, the growing hair bulb is partly protected by a state known as immune privilege. This means the follicle displays relatively low levels of certain immune-stimulating molecules, reducing the chance that it will be recognized as a target. The follicle can also produce local factors that dampen immune activity. This protection is especially relevant during anagen, when the follicle is metabolically active and vulnerable to immune surveillance.
In alopecia areata, that protection breaks down. Genetic susceptibility appears to prime the immune system for this misrecognition, and then inflammatory signaling amplifies the response. Once immune privilege is lost, follicular cells begin expressing molecules that attract and activate immune cells. CD8+ T cells gather around the bulb and release cytokines that interfere with normal follicular function. This immune attack does not typically kill the follicle outright, but it alters the signals that maintain anagen growth.
The follicle then prematurely shifts out of active growth. Instead of continuing to produce a normal hair shaft, it may enter catagen or a prolonged dormant state. The hair can become narrow, weak, and shed before reaching full length. Because the follicle remains structurally present, regrowth is biologically possible if immune activity subsides and follicular signaling normalizes. This reversibility is one reason alopecia areata is classified as non-scarring.
At the molecular level, several signaling pathways help sustain the disease process. Interferon-gamma can induce expression of inflammatory molecules in follicular cells, while JAK-STAT signaling transmits immune messages inside those cells. These pathways reinforce immune cell recruitment and maintain the abnormal environment around the follicle. The result is a self-perpetuating loop: immune activation disrupts follicle behavior, and the altered follicle environment further supports immune activation.
Structural or Functional Changes Caused by the Condition
The most important structural change in alopecia areata is not follicular destruction but functional suppression of hair growth. Histologically, affected follicles often show a dense lymphocytic infiltrate around the bulb, classically described as a “swarm of bees” pattern. This reflects immune cells clustered around the active growth region of the follicle. The inflammation is usually concentrated around anagen follicles, which helps explain why growing hairs are preferentially affected.
As the inflammatory process continues, the follicle shortens and miniaturizes in a reversible way. The hair bulb becomes less robust, matrix cell proliferation falls, and the hair shaft may narrow. Some hairs enter a dystrophic phase and break easily. Because the follicle remains alive, the skin surface usually stays smooth rather than scarred. There is no extensive replacement of follicles by collagen, and the sebaceous glands and surrounding skin architecture are generally preserved.
Functionally, the skin loses the ability to maintain normal hair density in the affected area. This can occur in patches or over broader regions depending on the extent of immune activation. The extent of visible hair loss reflects the number of follicles affected and the duration of the inflammatory state. In more extensive disease, the disruption can involve most or all scalp follicles, while in limited disease only a small number of follicles are suppressed.
Factors That Influence the Development of the Condition
Genetic predisposition plays a major role in alopecia areata. The condition clusters in families more often than expected by chance, and certain immune-related genes are associated with susceptibility. These genes often influence antigen presentation, lymphocyte activation, or cytokine signaling. In practical terms, inherited variation can make the immune system more likely to respond abnormally to follicular antigens.
Immune regulation is another major factor. Alopecia areata is more common in people who have other autoimmune conditions, which suggests shared immune mechanisms rather than a single isolated defect. The skin and hair follicle are influenced by the broader immune environment, so systemic immune activity can affect whether the follicle remains protected. However, the disease does not require a visible infection or injury to begin; it can arise from internal immune dysregulation alone.
Environmental influences may contribute as triggers in genetically susceptible people. Physical stress on the body, certain infections, or major physiologic changes have been reported in association with onset, although no single trigger explains most cases. These factors are best understood as potential stimuli that alter immune balance rather than direct causes of follicle loss. They may shift cytokine levels or change immune cell behavior enough to unmask the underlying susceptibility.
Hormonal influences are less central than in some other hair disorders, but the endocrine and immune systems interact. Hair follicles respond to a range of local and systemic signals, and any factor that changes inflammatory tone or follicular cycling can modify disease expression. Nutritional status may affect hair quality in general, yet alopecia areata is not caused by simple nutrient deficiency. The key mechanism remains immune-mediated disruption of the follicle.
Variations or Forms of the Condition
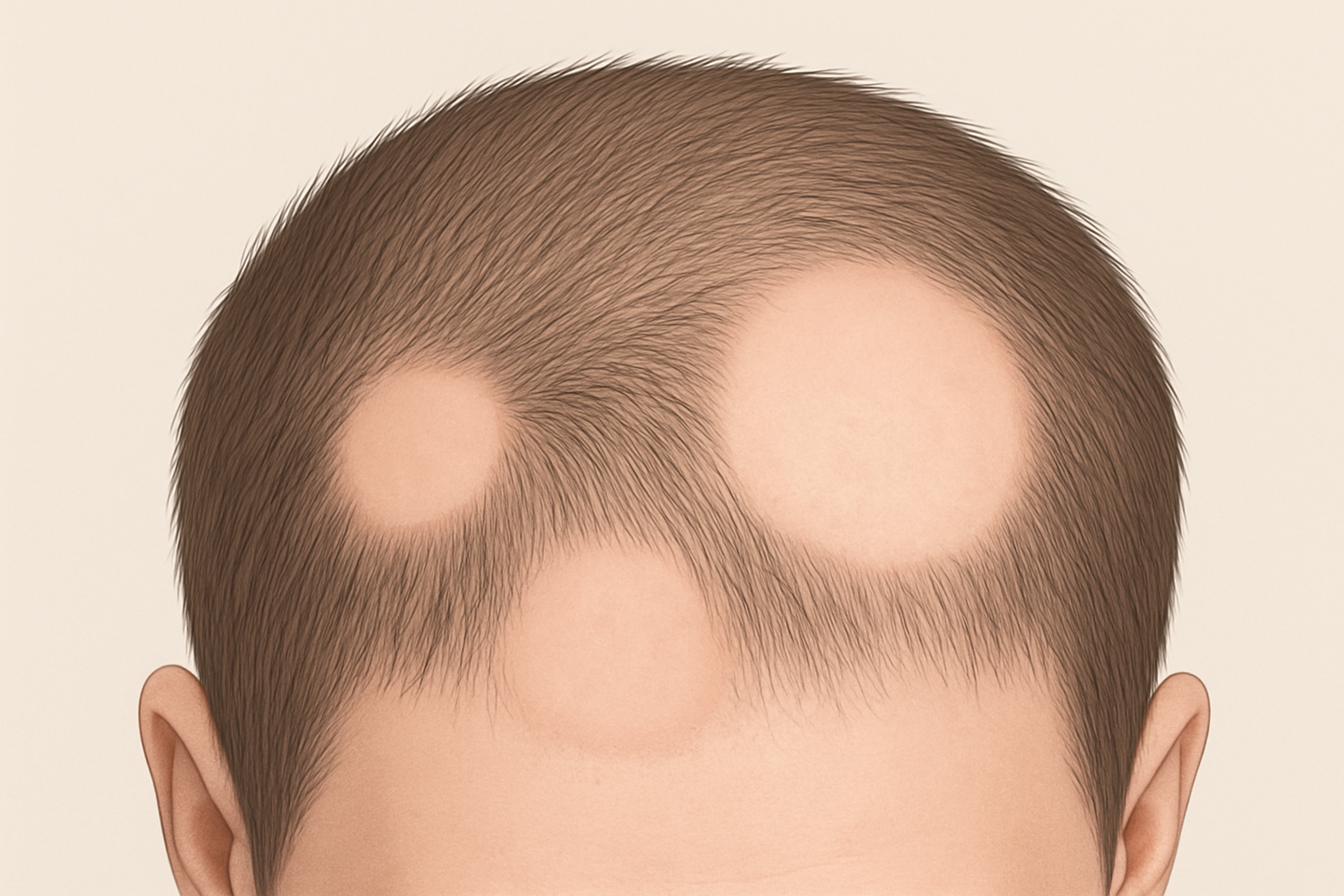
Alopecia areata appears in several clinical patterns that reflect differences in the intensity and distribution of immune attack. The most common form is patchy alopecia areata, in which one or more round or oval areas of hair loss develop on the scalp or elsewhere. In this form, immune activity is limited to selected groups of follicles, and neighboring follicles may remain unaffected.
When the immune response becomes more extensive, the disease may progress to alopecia totalis, involving complete or near-complete loss of scalp hair. In alopecia universalis, hair loss extends across the entire body, including eyebrows, eyelashes, and body hair. These more severe forms likely reflect broader immune targeting, stronger inflammatory signaling, or a failure of the follicle to restore immune privilege.
Some people experience ophiasis, a pattern in which hair loss affects the margins of the scalp in a band-like distribution. This pattern may reflect regional differences in follicular susceptibility or local immune environment. The disease can also vary in course, with single episodes, repeated relapses, or chronic persistent activity. These differences are not separate diseases but different expressions of the same underlying process of immune-mediated follicular suppression.
How the Condition Affects the Body Over Time
Over time, alopecia areata may remain limited to a small area, expand to involve multiple regions, or wax and wane unpredictably. The follicle can recover if immune pressure decreases, so regrowth is biologically possible even after substantial loss. In some cases, regrown hairs may initially differ in color or thickness because newly reactivated follicles do not immediately return to full normal cycling.
Persistent inflammation can alter the timing and quality of follicle cycling. Repeated immune attacks may keep many follicles from staying in anagen long enough to produce normal terminal hairs. This creates a chronic mismatch between the follicle’s capacity to grow hair and the immune system’s interference with that process. Even without scarring, prolonged disease can therefore produce sustained reduction in hair density and altered hair distribution.
The broader physiologic consequence is limited to the skin appendage in most cases, but the disease also reflects ongoing immune dysregulation elsewhere in the body. People with alopecia areata may have a higher likelihood of other autoimmune activity because the same immune imbalance can affect multiple tissues. The follicle itself may remain viable for years, yet repeated immune challenges can prevent stable return to normal growth.
Conclusion
Alopecia areata is an autoimmune disorder of the hair follicle in which immune cells disrupt normal hair growth without permanently destroying the follicle in most cases. The condition arises when immune privilege at the follicular bulb fails, allowing T-cell mediated inflammation and cytokine signaling to interfere with the hair cycle. The result is a non-scarring form of hair loss driven by immune dysregulation, altered follicular signaling, and premature interruption of anagen growth.
Understanding alopecia areata as a disorder of follicular immunology clarifies why it can appear suddenly, why it may reverse, and why its severity varies so widely. The central issue is not loss of skin structure but loss of immune control around a specialized skin organ. That biological framework explains the condition more accurately than a simple description of hair loss alone.