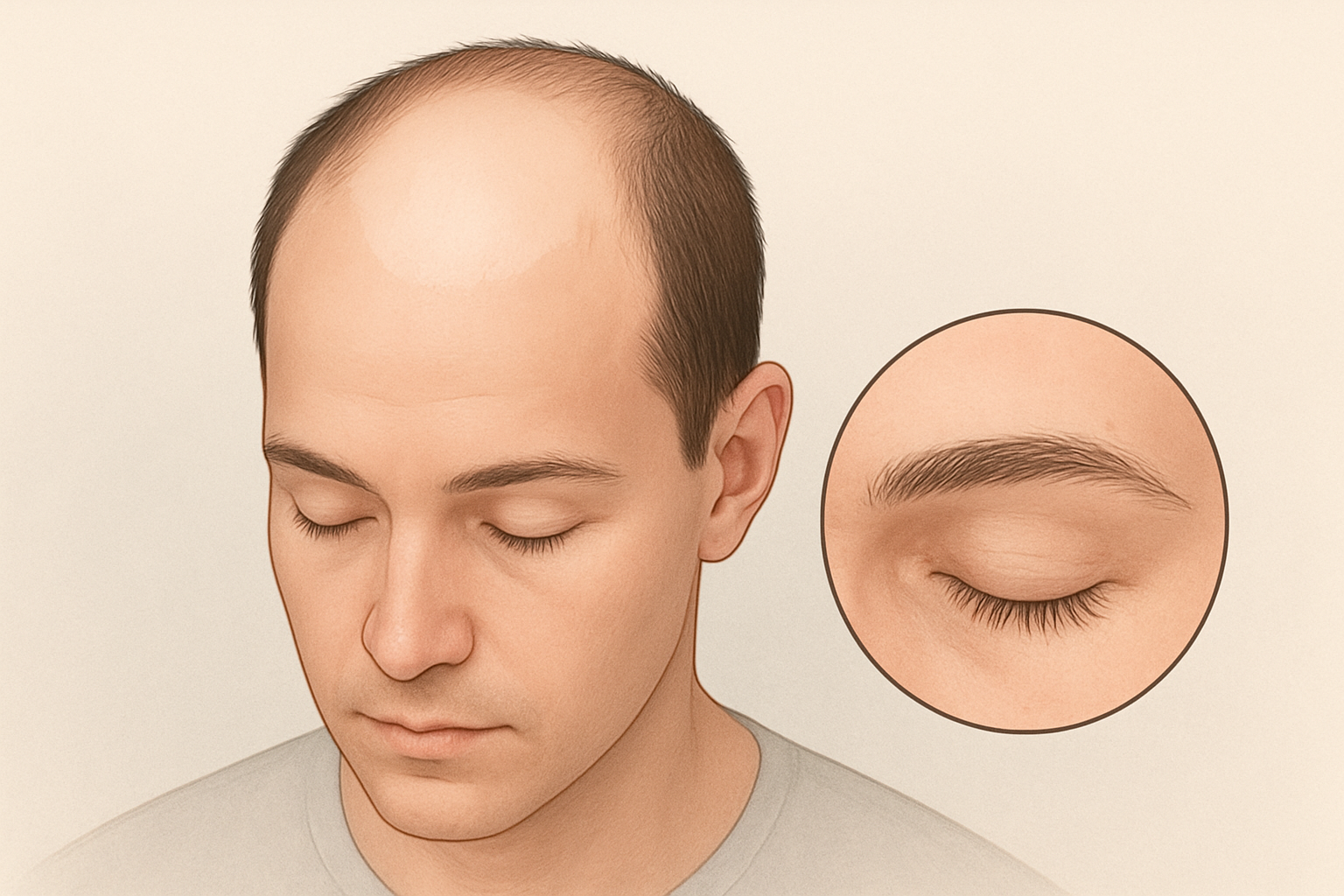
Introduction
The symptoms of Alopecia areata are most often sudden patches of hair loss, usually on the scalp, but they can also involve the eyebrows, eyelashes, beard, or other body hair. These symptoms arise because the immune system mistakenly targets hair follicles, interrupting normal hair growth and causing visible changes in the skin and hair shaft. In some people, the condition remains limited to a few small patches; in others, it progresses to more extensive loss of scalp or body hair. The pattern of symptoms reflects what happens inside the follicle when immune activity disrupts the hair growth cycle.
The Biological Processes Behind the Symptoms
Alopecia areata is primarily an immune mediated condition. Hair follicles normally cycle through phases of growth, regression, and rest, and during active growth they are relatively protected from immune attack. In Alopecia areata, that protection is lost. Immune cells, especially T lymphocytes, gather around the lower part of the follicle and release inflammatory signals that interfere with follicle function. This does not usually destroy the follicle permanently, but it pushes the follicle out of its normal growth phase and into a state where it stops producing a normal hair shaft.
The result is a form of non scarring hair loss. Because the follicle remains structurally intact, the skin often looks smooth rather than scarred or inflamed. The observable symptoms come from altered follicle biology: hairs break the cycle of normal growth, newly formed hairs become thinner or weaker, and the follicle may temporarily stop producing visible hair altogether. In some cases, the immune reaction also affects pigment production, which is why regrowing hairs may appear white or unpigmented at first.
Common Symptoms of Alopecia areata
The most characteristic symptom is one or more round or oval bald patches. These patches usually appear suddenly and may be noticed during grooming, showering, or brushing. The skin in the affected area is typically smooth, with little scaling or redness. This appearance reflects the fact that the follicles are functionally disrupted but the skin surface itself is not usually being destroyed. The immune attack is centered around the follicle rather than the epidermis, so the scalp may look normal apart from the missing hair.
Another common feature is hair shedding that seems more abrupt than in many other causes of hair loss. Hairs may fall out in clumps or become noticeably sparse over a short period. At the microscopic level, immune inflammation weakens the growing hair shaft and shortens the anagen, or growth, phase. As a result, hairs are released earlier than expected and stop contributing to visible coverage.
Some people notice exclamation point hairs, which are short hairs that are narrower at the base and thicker at the end. These are considered a classic sign of active disease. They form because inflammation weakens the follicle near the scalp, producing fragile hairs that taper where the shaft is damaged most. When such hairs break or shed, the remaining stump gives the impression of a mark with a thin base.
Itching, tingling, burning, or a mild tenderness can occur before or during active hair loss. These sensations do not arise in every case, but when present they suggest local inflammatory activity around the follicles. Immune signaling can stimulate nerve endings in the skin, producing sensory symptoms even when the surface looks relatively unremarkable. In many individuals, however, alopecia areata causes hair loss without pain or itching.
Changes in regrowing hair are also common. New hairs may appear fine, short, and white before gradually thickening and repigmenting. This reflects partial recovery of follicle function. Melanocytes, the cells that produce pigment, are particularly sensitive to the inflammatory environment, so pigment production may lag behind structural hair growth.
How Symptoms May Develop or Progress
Early symptoms often begin with a small, sharply defined patch of hair loss. The area may be discovered incidentally because the scalp skin usually remains intact and may not look inflamed. At this stage, the follicle is often entering an abrupt transition from active growth to a premature resting state, which is why the change can appear sudden rather than gradual.
As the condition progresses, one patch may enlarge or additional patches may appear. New lesions can develop in the same region or at distant sites. This pattern is driven by the spread or persistence of immune activity against multiple follicles. Because the underlying process is autoimmune rather than a local infection or injury, the pattern can shift unpredictably over time.
In some individuals, hair loss becomes more extensive. Multiple scalp patches may merge, or almost all scalp hair may be lost. In more severe forms, eyebrow, eyelash, beard, and body hair can also be affected. These broader patterns suggest a stronger or more sustained immune response, with follicular cycling disturbed across several hair bearing regions.
Symptoms may also fluctuate. Hair can regrow spontaneously, then shed again later. This relapsing pattern reflects the fact that follicle immune activity may wax and wane. When inflammatory signaling decreases, follicles can resume normal cycling. When immune activation returns, growth may halt again. Because the follicles are not usually scarred, repeated cycles of loss and regrowth are biologically possible.
Less Common or Secondary Symptoms
Some people develop nail changes alongside hair loss. These can include pitting, ridging, brittleness, or roughness of the nail surface. Nails and hair share some aspects of keratin biology, and the same immune dysregulation that affects the follicle may also influence nail formation. Nail symptoms are not universal, but when they appear they can indicate a broader immune impact on keratinized tissues.
Another less common feature is diffuse thinning rather than clearly defined bald patches. In this pattern, the immune effect may be less focal or more subtle, causing many hairs to shift into resting phases at once. Because the loss is spread out, the scalp may appear less dramatically patchy, even though the underlying follicular disturbance is similar.
Some individuals experience hair regrowth that initially lacks normal color or texture. Hairs may come back white, blond, or finer than before. This happens because pigmentation and shaft thickness recover at different rates. The follicle may resume producing hair before full melanocyte activity returns, and newly emerging fibers may be thinner until the growth environment normalizes.
Factors That Influence Symptom Patterns
The severity of immune involvement strongly shapes symptom expression. Limited follicular attack may produce one or a few small patches, while more widespread activity can lead to extensive scalp or body hair loss. The intensity and distribution of immune signaling influence how many follicles are pushed out of the growth cycle at any given time.
Age can affect how the condition appears. In younger individuals, patches may be noticed first on the scalp and can behave unpredictably over time. In adults, patterns may still be patchy, but associated nail changes or involvement of the beard and eyebrows may be more obvious in some cases. Age does not determine the mechanism, but it can influence which hair bearing areas are affected and how the pattern is perceived.
General immune status and related inflammatory conditions can also shape symptoms. Alopecia areata is more likely to occur in people with other immune mediated disorders, and that broader immune tendency can be associated with more persistent or recurrent follicular inflammation. The symptom pattern may therefore reflect not only the hair follicle itself, but the overall regulatory balance of the immune system.
Environmental or physiological stressors may influence when symptoms become visible, although they do not create the fundamental disease mechanism on their own. Illness, major stress, or other immune activating events can alter immune signaling and make follicular loss more likely to appear or recur. These influences affect timing and severity by shifting the immune environment in which follicles operate.
Warning Signs or Concerning Symptoms
Rapid expansion of hair loss over a short period can suggest a more active immune phase. When patches enlarge quickly or new areas appear in succession, it indicates that more follicles are being pushed out of the growth cycle. This pattern may precede more extensive loss, including involvement of eyebrows, eyelashes, or body hair.
Loss of eyelashes or eyebrows can be especially significant because these areas are more visible indicators of broader follicular involvement. Their appearance often means the immune process is affecting multiple types of hair follicles rather than remaining confined to one scalp patch. Since these follicles have different growth characteristics, their involvement suggests a more generalized inflammatory pattern.
Marked nail changes, such as pronounced pitting or brittleness, can also indicate more widespread disease activity. These findings reflect a stronger or more systemically expressed immune effect on keratin producing tissues. While not dangerous in themselves, they can accompany a broader inflammatory pattern.
Severe scalp sensitivity, redness, scale, or crusting is less typical for Alopecia areata and may indicate another process in addition to follicular immune attack. Because the classic condition usually preserves the skin surface, prominent inflammatory skin changes raise the possibility of overlap with another dermatologic disorder. The underlying physiology in such cases may extend beyond the usual follicle centered immune reaction.
Conclusion
The symptoms of Alopecia areata center on abrupt, non scarring hair loss with smooth bald patches, sometimes accompanied by exclamation point hairs, mild sensory symptoms, nail changes, and variable regrowth. These visible signs arise because immune cells disrupt the normal cycling of hair follicles rather than destroying them outright. The follicle enters a premature resting state, hair shafts weaken or shed, and pigment production may be temporarily altered. As a result, the condition produces a distinctive pattern of hair loss that can range from limited patchiness to more extensive involvement of scalp and body hair, with symptoms that often change as immune activity rises and falls.